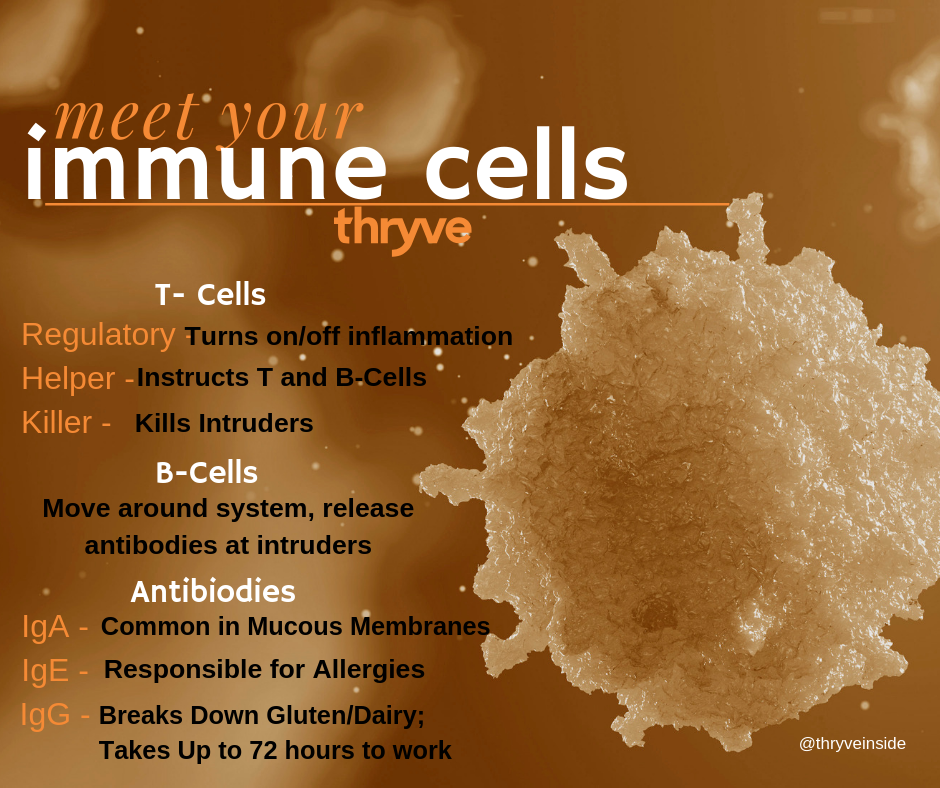
Innate vs. Adaptive Immune System. What’s the Difference?
Our body is such a complex system. Two main components have an impact on how this system works. In historical, scientific references, these all-powerful forces might be described as nature vs. nurture. Nothing is a better example of nature vs. nurture than our immune system. Most notably, we’re talking about the innate and adaptive immune system.
The human immune system is designed to protect us from the threat of foreign invaders. Unfortunately, the immune system we developed can only do so much. Our current lifestyle sets our immune system up to endure constant attack. Thankfully, our immune system can evolve to handle these situations. Let’s get to know both systems a little better.
How Do We Develop an Immune System?
We want to think that our parents, doctors, and nurses were the first living beings we’ve encountered in our lifetime. However, we met trillions of microbes inside of our mother’s womb as a zygote.
As a matter of fact, our mother’s microbes helped develop a fetus into an actual body. Their first line of action? Create our immune system!
Immunology of the Fetus
After around five weeks, a zygote develops a spleen 1. The spleen will be the first part of the body to secrete immune cells once the mother enters her second trimester.

Next up, the zygote will become an embryo. At this point, they will develop lymph nodes. Lymph nodes are essential for a properly functioning immune system. Fluids within these pathways help trap pathogens. That way, immune cells can come and wipe out the enemy.
Finally, the GI tract of the fetus is developed. This milestone will take place around the thirteen-week mark. Simultaneously, the first immune cells of the fetus start to form.
IgG Immune Cells in Utero
As you can tell, setting up an immune system is of the utmost importance for a fetus. It’s ingrained in our DNA to protect ourselves from potential threats. Our mother’s cells help make that happen.
A little after thirteen weeks, Immunoglobulin G (IgG) will pass the placenta and into the embryo.
One analysis found,
“Placental transfer of maternal IgG antibodies to the fetus is an important mechanism that provides protection to the infant while his/her humoral response is inefficient. IgG is the only antibody class that significantly crosses the human placenta 2.”
– Journal of Immunology Research
Yeah, we should be thanking our mom. This immune cell will eventually make up 75% of the antibodies in our body 3. It’s also the first steps in our development of the innate immune system.
Immune Cells in Breast Milk
When we are born, we are entering a whole new world. Life is not as cushy as it was in our mom’s womb.

In there, we just had to deal with the pathogens that were trying to ruin her intestinal flora.
Now, we have to deal with everyone else’s.
Babies are not as helpless as we like to believe. Their immune system is already in place.
However, they’re not fully developed. In fact, that’s going to be an ongoing process until they reach puberty.
Post-Birth Immune System Growth
An in-depth analysis looking at the development of the immune system from fetus to adulthood states,
“The young human child, even as the innate and adaptive immune systems start to mature, is at risk from many pathogenic viruses, bacteria, fungi and parasites 4. “
– Proc Biol Sci.
Their lacking immune system is why so many elementary school students have sick days. They’re only accustomed to the pathogens they met in womb and just have the immune cells their mother passed on to them.
As the analysis explained further,
“The immune system gradually matures during infancy. Critical early protection against many infectious diseases previously experienced by the mother is given by the passive IgG antibody transferred from the mother transplacentally and in milk. Once that fades away, young children become more vulnerable to infections, though by then better armed with the maturing innate and adaptive immune systems.”
– Proc Biol Sci.
Like they say; sometimes you have to get a bit dirty. Your child’s immune system must grow over time. However, it needs backup from familiar immune cells. That’s why breastfeeding can be so beneficial.

Immune cells and probiotics in breast milk help strengthen the child’s gut biome. In turn, they produce more immune cells. If you decide not to breastfeed, please consult a physician about ways to boost your child’s immune system naturally. This crucial time in their life is where your child relies on the innate immune system more than ever.
What is the Innate Immune System?
Our innate immune system is the “nurture” aspect of our immune system. These are the cells that act as our first line of defense. When you get a cold, these cells create the mucus to blow the germs out. If you get a cut, these cells cause that hot sensation at the site of the laceration.
You know your innate system is at work when you experience:

The initial reaction to an intruder from the innate immune system is to spark inflammation. Our immune cells try to kill off the foreign substance quickly with inflammation. Then, more immune cells put out the inflammation.
Common immune cells in our innate immune system include:
- Natural Killer Cells
- Mast Cells
- Eosinophils
- Basophils
- Phagocytic Cells (Macrophage, Neutrophils, Dendritic Cell)
When the innate immune system fails, inflammations continue. Long-term inflammation from immune cells may lead to autoimmune disease 5. In these moments, the adaptive immune system jumps into the thick of things.
What is the Adaptive Immune System?
Our adaptive immune system is more methodical than our innate immune system. The adaptive immune system takes note of long-term unwanted residents. From there, it constructs a battleplan to destroy these pathogens.
This “big picture” ideology is the “nature” aspect of our immune system. As the name implies, our adaptive immune system adapts. It alters for the ever-changing environments we enter and the revolving door of pathogens that end up in our system.
What’s excellent about adaptive immune systems are that they can eradicate the threat of disease forever. Let’s take chickenpox, for example.
As explained by the Mayo Clinic,
“Most people who have had chickenpox or have been vaccinated against chickenpox are immune to chickenpox. If you’ve been vaccinated and still get chickenpox, symptoms are often milder, with fewer blisters and mild or no fever. A few people can get chickenpox more than once, but this is rare 6.
– Mayo Clinic
The reason people tend not to get chickenpox twice is that our adaptive immune system creates antibodies. These antibodies are sort of like vaccines. Thanks to antibodies, the varicella virus (chickenpox) can’t survive in our system.
What Are Antibodies?
Antibodies are Y-shaped proteins that latches onto intruders, inhibiting them from taking over the system. They are formulated to target specific pathogens. These defense mechanisms are secreted from B-cells of our adaptive immune system.
B-cells study the target for a while. Then, they call on inflammatory cells to eradicate the problem. However, each intruder needs a specific formula to destroy them. So, the adaptive immune system works to crack that code. Once they do, they create the perfect elixir to get rid of the threat for good. That plan of attack is antibodies.
Want to know what else is an antibody? The IgG cell we talked about before. That’s right, your mother’s immune system equipped you with antibodies to start you on this journey. Now we’ve come full circle. Thanks for exploring your innate and adaptive immune system with us!
Give your immune system a break. Help them out with probiotics. Get your gut tested with Ombre today and rebuild intestinal flora that produce immune cells.
Resources
- 1 “Immune System Development.” Embryology, 19 Sept. 2019, embryology.med.unsw.edu.au/embryology/index.php/Immune_System_Development.
- 2 Palmeira, Patricia, et al. “IgG Placental Transfer in Healthy and Pathological Pregnancies.” Journal of Immunology Research, Hindawi, 1 Oct. 2011, www.hindawi.com/journals/jir/2012/985646/.
- 3 Gocki, J., & Bartuzi, Z. (2016). Role of immunoglobulin G antibodies in diagnosis of food allergy. Postepy dermatologii i alergologii, 33(4), 253–256. doi:10.5114/ada.2016.61600.
- 4 Simon, A. K., Hollander, G. A., & McMichael, A. (2015). Evolution of the immune system in humans from infancy to old age. Proceedings. Biological sciences, 282(1821), 20143085. doi:10.1098/rspb.2014.3085.
- 5 Duan, L., Rao, X., & Sigdel, K. R. (2019). Regulation of Inflammation in Autoimmune Disease. Journal of immunology research, 2019, 7403796. doi:10.1155/2019/7403796.
- 6 “Chickenpox.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 27 Feb. 2019, www.mayoclinic.org/diseases-conditions/chickenpox/symptoms-causes/syc-20351282.